Preventive Health
With Dzeus you can get check-ups, prevent illnesses and receive personalized medical recommendations, all from the comfort and privacy of your own home.
Available Consultations
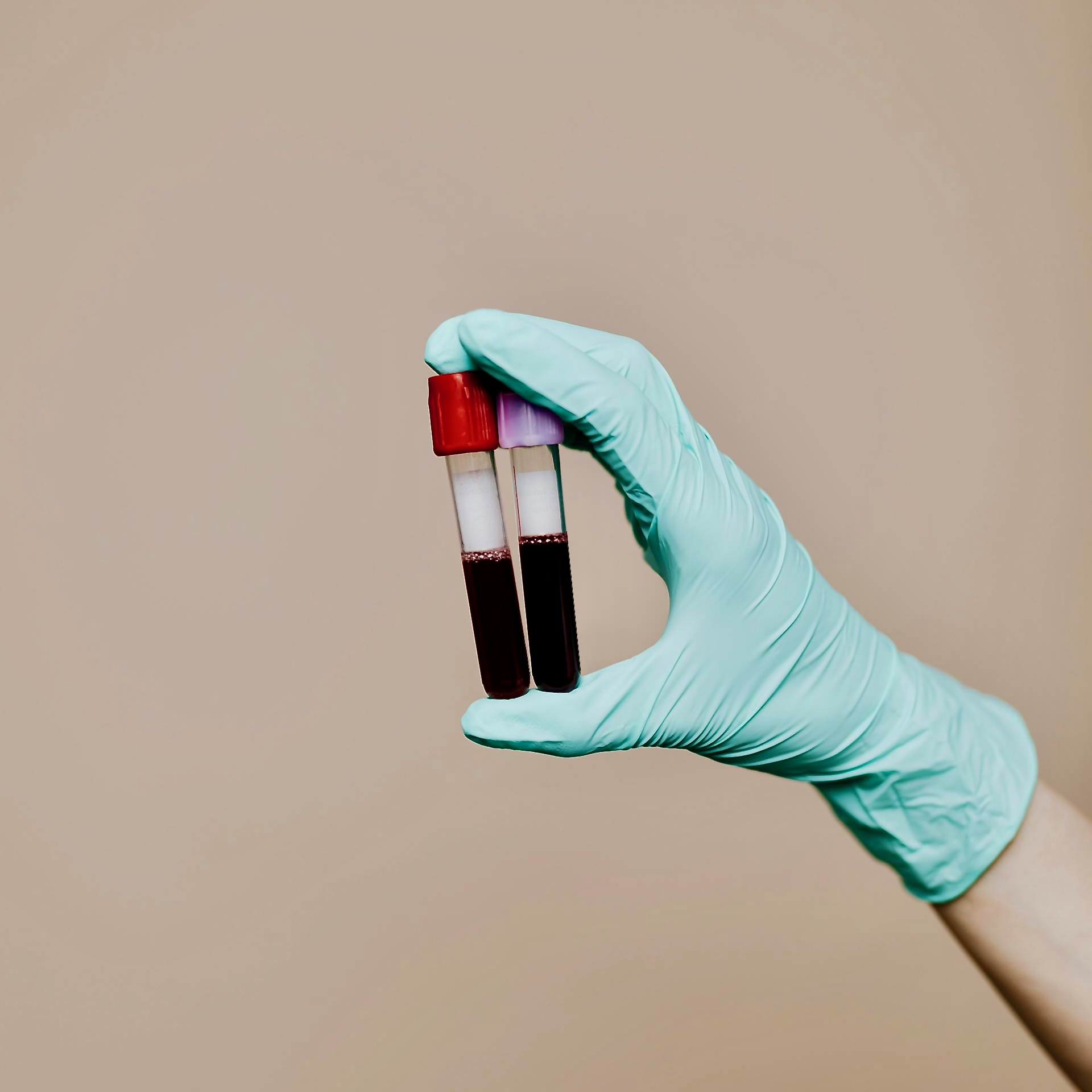
Lab Tests
• Preventive Health
›

Lab Tests
Referrals starting at $10